Asthma Facts
Asthma Facts, Figures, and Stats
Asthma is one of the most common and costly diseases in the United States. The groups most affected by asthma are people with lower incomes, older adults, and people who are Black or Indigenous. These groups have the highest asthma rates, hospital visits/stays, and deaths.
On this page:
What is asthma? What happens in the lungs?
What are the symptoms of asthma?
How common is asthma? What are the prevalence rates?
What are the rates of asthma attacks in children?
What are the rates of asthma attacks in adults?
How many people seek medical care for asthma?
How many people die from asthma?
What are the costs of asthma?
Why do asthma rates vary based on race, ethnicity, sex, gender, or age?
What Is Asthma?
Asthma is a chronic (long-term) disease that causes inflammation and swelling of the airways.
- In lungs with asthma: the small muscles around the airways to squeeze and tighten, the inside of the airways swell, and extra mucus clogs the airways.
- There is no cure for asthma, but asthma attacks can be prevented and treated to help people have better quality of life.
- Asthma can be managed and controlled, but without appropriate treatment, it can cause permanent lung damage, reduced lung function, and death.
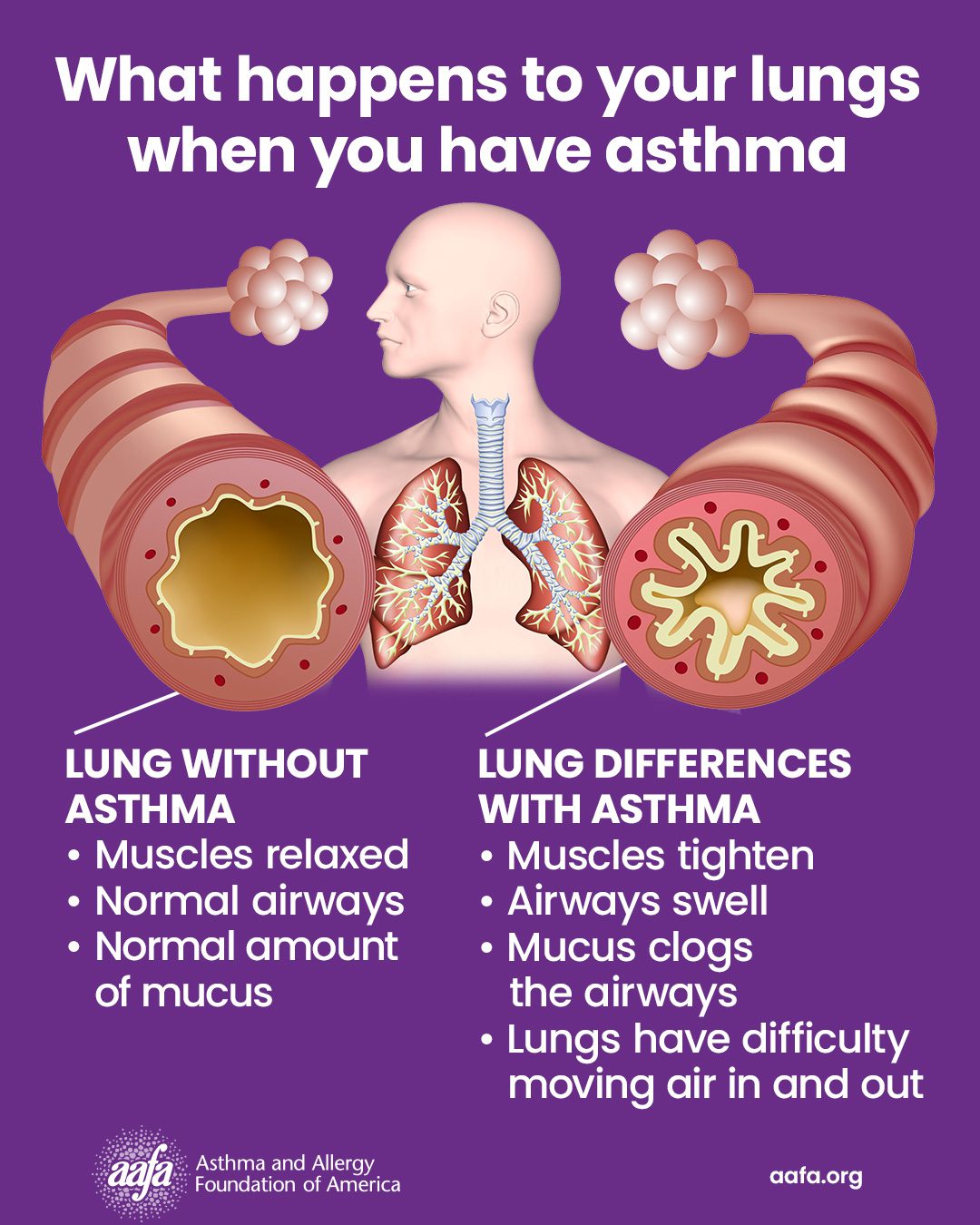
What happens in your lungs when you have asthma
Asthma causes the airways to narrow and get clogged. Asthma medicines treat the swelling and squeezing of the airways.
What Are the Symptoms of Asthma?
Asthma symptoms include trouble breathing (shortness of breath, shallow breathing, or fast breathing), wheezing, coughing, and tightness or pain in the chest.
- Signs of an asthma emergency include trouble breathing that makes it hard to talk or walk; color changes on skin, lips, tongue, fingertips from not getting enough air; chest sucks in between neck, chest plate, or ribs when breathing in.
Common asthma symptoms
Common asthma symptoms include coughing, wheezing, shortness of breath, and chest tightness or pain. Symptoms may wake you up at night. You may not have all these symptoms.
How Common Is Asthma?
Nearly 28 million people in the U.S. have asthma. This equals about 8% (8 out of 100) people.1,2
Asthma in Adults:
- About 23 million U.S. adults (or about 9 out of 100) ages 18 and older have asthma.1
- Adults in the U.S. with asthma:
Ages 20-24: 2 million
Ages 25-34: 3.5 million
Ages 35-64: 10 million
Ages 65+ : 4 million - Asthma rates are highest in Black and Indigenous adults in the U.S.1
- About 3 million Black adults (or about 10 out of 100) have asthma.
- About 347,000 Indigenous adults (or about 10 out of 100) have asthma.
- About 18 million White adults (or about 9 out of 100) have asthma.
- About 3 million Hispanic adults (or about 7 out of 100) have asthma.
- About 823,000 Asian adults (or about 5 out of 100) have asthma.
- Asthma is more common in female adults than male adults. 1
- Around 11% (11 out of 100) of female adults have asthma.
- 6% (6 out of 100) of male adults have asthma.
- Asthma is more common in adults living below the federal poverty level than adults with higher incomes.1
- About 12 out of 100 adults living below the federal poverty level ($15,060 in 2024) have asthma, compared to about 8 out of 100 adults who made $30,120 or more in 2024.
- Asthma is more common in gay and bisexual adults compared to straight adults.3
- A 2022 report found that 11 out of 100 straight men had asthma, compared to 13 out of 100 gay men and 15 out of 100 bisexual men.3
- The same report found that 14 out of 100 straight women had asthma, compared to 21 out of 100 lesbian women and 24 out of 100 bisexual women.3
Asthma in Children:
- There are close to 5 million U.S. children (or about 7 out of 100) under the age of 18 with asthma.2
- Asthma is a top chronic disease in U.S. children.4
- Only tooth decay (cavities) is more common than asthma. 5
- Long COVID affects 4% (or 4 out of 100) which equals about 3 million children.6
- Black children are nearly 2 times more likely to have asthma compared to White children.
- About 1 million (or 11 out of 100) Black children have asthma.
- About 3 million (or 6 out of 100) White children have asthma.
- About 1 million Hispanic children (or about 7 out of 100) have asthma.
- About 163,000 Asian children (or about 4 out of 100) have asthma. 2
- Childhood asthma rates are close between sexes, with rates being a little higher in male children than female children.
- Around 7% (7 out of 100) of male children have asthma, compared to 6% (6 out of 100) of female children.2
What Are the Rates of Asthma Attacks in Children?
- Most children with asthma have one or more asthma attacks per year.
- In 2022, over half (53%, or 53 out of 100) of children under the age of 18 who had asthma reported having one or more asthma attacks in the past year.7
- In 2022, 68 out of 100 children under the age of 5 with asthma had an asthma attack.7
- Even though asthma is controllable, it is estimated that 44 out of 100 children with asthma have uncontrolled asthma.8
- Only about half of children with asthma have been given an asthma action plan.9
Asthma stats in children
Almost half of kids with asthma have uncontrolled asthma which can lead to missed school days, hospital stays, and lower quality of life.
What Are the Rates of Asthma Attacks in Adults?
- In 2022, 40 out of 100 adults aged 18 and older who had asthma reported having one or more asthma attacks in the past year. This equals 8 million people. 7
- Asthma attack rates are higher in adults with lower income and wealth.7
- In 2022, 45 out of 100 adults with asthma living below the federal poverty level ($13,590 in 2022) had an asthma attack, compared to 37 out of 100 adults who made $61,155 or more.7
- Asthma attack rates are higher in Hispanic adults compared to non-Hispanic adults.7
- In 2022, 44 out of 100 Hispanic adults with asthma had an asthma attack, compared to 40 out of 100 non-Hispanic White adults with asthma and 38 in 100 Black adults with asthma.7
How Many People Seek Medical Care for Asthma?
- In 2019, asthma accounted for nearly 5 (4.9) million doctors’ office visits.10
- In 2020, asthma accounted for nearly 100,000 (94,560) discharges from hospital inpatient care and almost 1 million (986,453) emergency department visits.11
- Black people in the U.S. are nearly 6 times more likely than White people in the U.S. to visit the emergency department due to asthma.
- In 2020, 83 out of 100 Black people with asthma went to the emergency department for asthma, compared to 14 out of 100 White people with asthma.11
- Black people in the U.S. are also nearly 5 times more likely than White people in the U.S. to be hospitalized for asthma.
- In 2020, 7 out of 100 Black people with asthma were hospitalized for asthma, compared to 2 out of 100 White people with asthma.11
- Young children are more likely than older adults to visit the emergency department for asthma.
- In 2020, 42 out of 100 children with asthma aged 0-4 years went to the emergency department for asthma, compared to 13 out of 100 adults with asthma over the age of 65.11
- Young children are also more likely to be hospitalized for asthma.
- In 2020, 6 out of 100 children with asthma aged 0-4 years were hospitalized, compared to 3 out of 100 people with asthma over the age of 5.11
- Boys are more likely to visit the emergency department for asthma compared to girls, but women are more likely to visit the emergency department for asthma compared to men.11
- In 2020, 43 out of 100 boys with asthma went to the emergency department for asthma compared to 30 out of 100 girls with asthma
- In the same year, 33 out of 100 women with asthma went to the emergency department for asthma compared to 22 out of 100 men with asthma.
- Asthma symptoms worsen in about 40 out of 100 people with asthma who are pregnant. And at least 20 out of 100 will have asthma flares during pregnancy that require medical attention.12
Doctor visits for asthma
Sick visits for worsening asthma symptoms plus routine health care appointments for asthma management lead to 5 million doctor visits per year.
Emergency room visits for asthma
Asthma may lead to a medical emergency. If you have asthma, be sure to know the signs and symptoms of a severe asthma attack and when to seek emergency help.
How Many People Die from Asthma?
- On average, 9 to 11 people in the U.S. die from asthma each day. Nearly all of these deaths are avoidable with the right treatment and care.
- In 2024, 3,279 people died from asthma. 13
- In 2020, deaths due to asthma rose for the first time in 20 years. 14 This increase may have been due to the COVID-19 pandemic (before vaccination was available).
Deaths from asthma are preventable
If you have asthma, you can reduce your risk of death by following your asthma action plans, taking asthma medicines as prescribed, reducing exposure to your triggers, and getting medical help if you have asthma symptoms more than twice a week.
- The people who have the highest rates of dying from asthma are adults, female, and/or Black.
- Adults are 6 times more likely to die from asthma than children.
- In 2024, 12 out of 1 million deaths among adults were due to asthma, compared to 2 out of 1 million deaths among children.13
- Senior adults age 85 and over have the highest death rates due to asthma.
- In 2024, 83 out of 1 million deaths among people age 85 and over were due to asthma, compared to 27 out of 1 million deaths among people age 75-84.13
- Female adults are more likely to die from asthma than male adults.
- In 2024, 14 out of 1 million deaths among female adults were due to asthma, compared to 9 out of 1 million deaths among male adults. 13
- Black people in the U.S. are more than 2 times more likely to die from asthma than White people in the U.S.
- In 2024, 19 out of 1 million deaths among Black people were due to asthma, compared to 9 out of 1 million deaths among White people.13
- When sex is factored in, Black females have the highest rate of fatality due to asthma. Black females are more than 3 times more likely to die from asthma than White males.
- In 2024, 20 out of 1 million deaths among Black females were due to asthma, compared to 6 out of 1 million deaths among White males. 13
What Are the Costs of Asthma?
- Asthma is one of the most common and costly diseases in the United States.
- Adjusted for inflation, the estimated economic cost of asthma will be at least $118 billion in 2026.
- From 2008-2013, the annual economic cost of asthma was $82 billion – including medical costs, deaths, and loss of work and school days:15
- $3 billion in losses due to missed work and school days
- $29 billion due to asthma-related mortality
- $50.3 billion in medical costs
- Asthma is one of the top reasons people with asthma miss work or school. On average, people with asthma miss 2 more days of work or school each year than people without asthma.16
- Medical costs for people with asthma are estimated to be $3,266 higher per year (in 2015 U.S. dollars) compared to medical costs for people without asthma.15
- In 2024, the average retail price of an albuterol inhaler was $98.17
- Researchers estimate that from 2019-2038, the cost of uncontrolled asthma will be nearly $964 billion.18
- From 2014-2018, Medicare spent over $50 billion on inhalers.19
Cost of uncontrolled asthma
Uncontrolled asthma causes a significant financial burden on individuals, caregivers, and the United States.
Why Do Certain Groups of People Have Higher Rates of Asthma, Asthma Attacks, or Asthma Deaths?
Structural inequities (e.g. systemic racism, income and wealth inequities) and social drivers largely drive disparities in asthma. Factors such as genetics and individual behaviors contribute less to asthma disparities.
- Structural inequities (determinants) such as systemic racism, segregation, sexism, inequitable wealth distribution, labor markets, education systems, housing policies and availability, discriminatory policies, and climate change
- Social drivers (determinants) such as socioeconomic status, education quality, neighborhood and living environment, employment, social support networks, and access to health care
- Biological drivers (determinants) such as genes and ancestry
- Behavioral drivers (determinants) such as tobacco use and adherence to medicines
Racial and Ethnic Differences in Asthma Rates
- Racial and ethnic differences in asthma rates, attacks, emergencies, and deaths are caused by complex factors including systemic racism, gentrification, segregation, medical bias, and discriminatory policies that affect wealth accumulation, education quality, and employment.
Causes of asthma disparities
Asthma is greatly influenced by living conditions (social, physical, and environmental). People who live in poverty, and/or people who are Black, Puerto Rican, or Indigenous have higher asthma rates.
Sex and Gender Differences In Asthma Rates
- Sex and gender differences in asthma rates, attacks, emergencies, and deaths are largely caused by complex factors including systemic sexism, medical bias, and discriminatory policies that affect wealth accumulation, education quality, and employment. But biological factors related to sex may also influence asthma.
- Male children are more likely to have asthma than female children. This trend reverses in adulthood, where female adults are more likely to have asthma than male adults.1,2
- Some studies suggest this trend reverses because of the effects of testosterone on lung cells. Testosterone, a male sex hormone, has been found to decrease the swelling of the airways in asthma.21
Gender differences in asthma
Male children are more likely than female children to have asthma. This changes in adulthood and more females have asthma as adults.
Age Differences In Asthma Rates
- Age differences in asthma rates, attacks, emergencies, and deaths are caused by systemic structural, social, and biological factors.
- As people age, the risk of dying from asthma increases.
- Higher mortality rates in older adults are due to: underdiagnosis, co-occurring chronic conditions, use of medications that may worsen asthma, reduced lung function, immune system weakening, exposure to respiratory infections, inability to afford medical care, impaired cognitive function, and difficulty using inhalers due to arthritis.
Closed
References
- National Center for Health Statistics. 2024 NHIS Adult Summary Health Statistics. Data accessed February 19, 2026. Available from https://data.cdc.gov/d/25m4-6qqq
- National Center for Health Statistics. 2024 NHIS Child Summary Health Statistics. Data accessed February 19, 2026. Available from https://data.cdc.gov/d/wxz7-ekz9
- Heslin, K., & Alfier, J. (2022). Sexual Orientation Differences in Access to Care and Health Status, Behaviors, and Beliefs: Findings from the National Health and Nutrition Examination Survey, National Survey of Family Growth, And National Health Interview Survey. National Health Statistics Reports, 171. https://www.cdc.gov/nchs/data/nhsr/nhsr171.pdf
- Ferrante, G., & La Grutta, S. (2018). The Burden of Pediatric Asthma. Frontiers in Pediatrics, 6. https://doi.org/10.3389/fped.2018.00186
- National Institute of Dental and Craniofacial Research. (2019). Dental caries (tooth decay) in children ages 2 to 11 years. National Institutes of Health. https://www.nidcr.nih.gov/research/data-statistics/dental-caries/children
- Mandel, H., Yoo, Y. J., Allen, A. J., Abedian, S., Verzani, Z., Karlson, E. W., Kleinman, L. C., Mudumbi, P. C., Oliveira, C. R., Muszynski, J. A., Gross, R. S., Carton, T. W., Kim, C., Taylor, E., Park, H., Divers, J., Kelly, J. D., Arnold, J., Geary, C. R., Zang, C., … Moffitt, R. A. (2025). Long COVID Incidence Proportion in Adults and Children Between 2020 and 2024: An Electronic Health Record-Based Study From the RECOVER Initiative. Clinical Infectious Diseases, 80(6), 1247–1261. https://doi.org/10.1093/cid/ciaf046
- Centers for Disease Control and Prevention. (2024). 2022: Percentage of Persons Who Had Asthma Attack by Age (NHIS). Asthma Data; U.S. Department of Health and Human Services. https://www.cdc.gov/asthma-data/nhis/2022-percentage-persons-asthma-attack-age.html
- National Asthma Control Program. (2022). Uncontrolled Asthma Among Children With Current Asthma, 2018–2020. National Center for Environmental Health. https://archive.cdc.gov/#/details?url=https://www.cdc.gov/asthma/asthma_stats/uncontrolled-asthma-children-2018-2020.htm
- Centers for Disease Control and Prevention. (2022). Asthma Self-Management Education Among Children With Current Asthma – United States, 2018. U.S. Department of Health and Human Services. https://www.cdc.gov/asthma/asthma_stats/asthma-children-self-managed-edu_2018.html
- National Center for Health Statistics. (2022). National Ambulatory Medical Care Survey: 2019 National Summary Tables. U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. https://www.cdc.gov/nchs/data/ahcd/namcs_summary/2019-namcs-web-tables-508.pdf
- Agency for Healthcare Research and Quality. (2023). Healthcare Cost and Utilization Project 2020 Healthcare Use Data. U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. https://www.cdc.gov/asthma/healthcare-use/2020/data.htm
- Murphy, V. E., Gibson, P. G., & Schatz, M. (2023). Managing Asthma During Pregnancy and the Postpartum Period. The Journal of Allergy and Clinical Immunology: In Practice, 11(12), 3585–3594. https://doi.org/10.1016/j.jaip.2023.07.020
- National Center for Health Statistics. National Vital Statistics System: Mortality (2018-2024). U.S. Department of Health and Human Services, Centers for Disease Control and Prevention. https://wonder.cdc.gov/ucd-icd10-expanded.html
- CDC National Asthma Control Program (NACP). (2023). Asthma Surveillance in the United States, 2001–2021. National Center for Environmental Health, Centers for Disease Control and Prevention. https://www.cdc.gov/asthma/asthma-prevalence-us-2023-508.pdf
- Nurmagambetov, T., Kuwahara, R., & Garbe, P. (2018). The Economic Burden of Asthma in the United States, 2008–2013. Annals of the American Thoracic Society, 15(3), 348–356. https://doi.org/10.1513/annalsats.201703-259oc
- Song, H. J., Blake, K. V., Wilson, D. L., Winterstein, A. G., & Park, H. (2020). Medical Costs and Productivity Loss Due to Mild, Moderate, and Severe Asthma in the United States. Journal of Asthma and Allergy, 13, 545–555. https://doi.org/10.2147/JAA.S272681
- The Conversation. (2024, March 10). Why Asthma Medication Is So Expensive in the U.S. U.S. News & World Report. https://www.usnews.com/news/healthiest-communities/articles/2024-03-10/why-asthma-medication-is-so-expensive-in-the-u-s
- Yaghoubi, M., Adibi, A., Safari, A., FitzGerald, J. M., & Sadatsafavi, M. (2019). The Projected Economic and Health Burden of Uncontrolled Asthma in the United States. American Journal of Respiratory and Critical Care Medicine, 200(9), 1102–1112. https://doi.org/10.1164/rccm.201901-0016oc
- Thomas, A., Haddad, I., & Hoskere, G. (2021). Trends in Inhaler Prescriptions and Associated Cost in the United States From 2014 to 2018: An Analysis From the Medicare Part D Database. Cureus, 13(2), e13498. https://doi.org/10.7759/cureus.13498
- Sistani, F., Reed, R. M., Shah, C. H., & Zafari, Z. (2021). Trends in Medicaid spending on inhalers in the United States, 2012-2018. Journal of Managed Care & Specialty Pharmacy, 27(12), 1744–1749. https://doi.org/10.18553/jmcp.2021.27.12.1744
- McKernan, K. E., Pilier, E. H., & Newcomb, D. C. (2026). Sex Differences in Asthma Pathogenesis. Immunological Reviews, 337(1). https://doi.org/10.1111/imr.70100